What are the incidence of burns?
How many require ER visits?
survival rate?
- 1.25 million burns annually
- 486,000/year in US require ER visits
- 40,000 hospitalized
- 30,000 admitted to a specialized burn center
- Incidence of burns has decreased secondary to education on prevention and safety regulations
- survival rate 96.8%
What are the different types of urns?
What factors may indicate an inhalational burn?
- Electrical
- Chemical
- Inhalational
- Burned within a closed airspace
- somebody who lost sonsciousness at the scene
- cinged nose hairs
- Thermal (most common)
What are the mortality rates for burns?
Who has increased risk of mortality from burns?
- LD50 is burn size >90% TBSA
- approx. 3,240 die from fire/smoke inhalation injury
- 2,855 from residential fires
- 300 from motor vehicle or aircraft
- ~75% of deaths occur at the scene or during transport
- ~35% burn victims <17 years old
- Increased mortality:
- older age (>60 years)
- >40% TBSA
- inhalational injury
What are the most common causes of death to a burn patient?
- Infection
- starvation
- **Increased survival thanks to early debridement of burns and early and continued nutritional support
What are the functions of the integumentary system?
What are the layers of the integumentary system?
- Integumentary system is largest organ
- protection
- containment
- heat regulation
- sensation
- vitamin D
- Layers:
- Epidermis- top layer
- avascular
- Dermis- second layer
- vascular with afferent nerve endings
- Fascia
- Epidermis- top layer
How are burns categorized?
- *Categorized based on depth and body surface area
- 1st degree- epidermis only
- heals spontaneously
- 2nd degree-
- Superficial partial thickness- basement membrane of dermis is intact
- does not usually require grafting
- deep dermal- basement membrane of dermis is not intact
- does require grafting
- Superficial partial thickness- basement membrane of dermis is intact
- 3rd degree- “full thickness”
- burn extends into subcutaneous tissue
- will need grafting
- 4th degree- muscle, fascia, bone
- can result in limb loss
Know the chart for 1st, 2nd, and 3rd degree burns:
depth
how wound looks
causes
level of pain
healing time
scarring

What is the rule of 9’s?
- The method used to calculate body surface involved in a burn.
- Head and neck = 9%
- Each upper extremity = 9%
- each lower extremity = 18%
- anterior trunk = 18%
- posterior trunk = 18%
- perineum = 1%
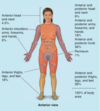
Why is the rule of nines inaccurate in calculating TBSA in children?
- because children have proportionally bigger head and trunk
- a small error in estimation of TBSA can cause a large change in resuscitation plan
What is the pathophysiology that occurs after a burn?
- SIRS
- Every system is affected
- Necrotic area and ischemic area
- ischemic area can potentially be saved with adequate resuscitation
- First minutes to hours:
- burned tissue releases inflammatory and vasoactive mediators
- histamine, prostaglandins, kinins, leukotrienes, thromboxane, and NO
- burned tissue releases inflammatory and vasoactive mediators
- Later:
- reperfusion injury- will produce reactive O2 species that will cause further damage and and propagate the immune response
What is significant about the zone of stasis?

- The zone of stasis is the area that can be salvaged with the appropriate resuscitation
- without adequate resuscitation the zone of stasis will be lost
What happens with electrical burns?
- Devastating injuries to bones, blood vessels, muscle and nerves
- Extent of tissue damage is based on voltage and duration
- Most damage concentrated at entry and exit points
- 10-46% have cardiac arrhythmias and maybe damage to myocardium
- Massive muscle damage will lead to renal failure d/t myoglobinemia
Chemical burns:
usual cause?
what does it do?
treatment?
- Usually caused by occupational injury
- The chemical causes a reaction with tissue proteins and cellular components that leads to tissue destruction
- Treatment: Must neutralize!
- copious irrigation
Thermal burns:
Who is usually affected?
- Scald injuries account for up to 70% of burns in children < 4 years old
- Children >5 years usually have flame burns
- 15-20% of burns are NAT caused by abuse or neglect
Inhalational injury:
symptoms
usual causes
- Symptoms:
- hoarseness
- sore throat
- dysphagia
- hemoptysis
- tachypnea
- accessory muscle usage
- wheezing
- carbonaceous sputum
- increased CO levels
- Causes:
- thermal burns, likely in a closed space.
- suspect if pt was unconscious at the scene
What are the three types of inhalational injuries?
- Upper airway injuries
- inhalation of superheated air/steam
- may spare lower airway d/t reflexive vocal cord closure if dry heat, less likely with steam
- Lower airway/parenchymal
- soot particle/chemical inhalation
- will cause massive bronchospasm
- Metabolic asphyxiation- CO, etc
What is the flow of the pathophysiology of an inhalation injury?
(small flow chart)
- the Conversion of xanthine oxidase causes the breakdown of purines to uric acid which creates reactive oxygen species
- The Reactive oxygen species combine with nitrous oxide(??), increase the microvascular pressure and the permeability to protein
- Neutrophils will be stiff and non-deformable b/c they are injured. This causes further release of oxygen radicals and further propagates the injury

Describe the large complicated flow chart of the pathophysiology of an inhalational injury.

What are the indications for early tracheal intubation after an inhalation injury?

When should you suspect CO poisoning?
How does CO affinity for Hgb compare to O2?
What does CO do to pH?
- Suspect CO poisoning with inhalational injuries
- dectect it with arterial COHgb levels
- Severity of symptoms will correlate with COHgb levels
- >30% COHgb requires high FiO2 to reduce half life
- always provide high FiO2 until it is proven the person does NOT have an inhalational injury/CO poisoning
- CO has 200 times greater affinity for hemoglobin than oxygen
- CO causes metabolic acidosis
How does CO affect the oxyhemoglobin dissociation curve?
How does CO interact with myoglobin?
How does CO affect SpO2?
- CO causes LEFT shift on oxy-hgb dissociation curve, reducing the oxygen release from the hgb.
- CO has a greter affinity for myoglbin than for hgb
- CO binding to cardiac myoglobin leads to myocardial depression, hypotension, and arrhythmias
- CO causes falsely elevated pulse oximetry readings
When would you see cherry red colored blood?
If carboxyhemoglobin level is >40%
What are the symptoms of CO poisoning?
(chart)
0-10%
10-20%
20-30%…

What does cyanide poisoning do?
What are the symptoms of cyanide poisoning?
What is the antidote and how does it work?
- Cyanide poisoning leads to tissue hypoxia by blocking the intracellular use of oxygen
- it binds to the terminal cytochrome on the exectron transport chain
- result is hypoxia, lactic acidosis, and elevated mixed venous oxygen saturation
- Symptoms:
- LOC
- mydriasis (dilated pupils)
- sz
- hypotension
- tachypnea then apnea
- increased lactate levels
- Antidote: Hydroxocobalamin (vit B 12)
- actively binds cyanide by forming cyanocobalamin
- directly excreted in kidney
What materials give off CO?
What materials give off cyanide?
(table)

What pharmacokinetic changes will you see in a pt during burn shock?
What about during the hypermatabolic phase?
- Burn shock: generally decreased requirements
- reductions in renal and hepatic blood flow
- prolonged rate of drug distribution
- prolonged onset of clinical effects
- Hypermetabolic phase: generally increased requirements
- decreased albumin
- increased a1-acid glycoprotein
- denervation phenomenon with spreading of acetylcholine receptors (no succ!)
- increased nicotinic acetylcholine receptors and decreased function
What are some considerations for these drugs in a patient with major burns? (table)
fluids
succs
NDMR
IV anesthetics
inhalation agents
beta blockers
insulin


