What are the Cardiovascular effects of neuraxial anesthesia?
Treatment?
- Sympathecomy causes vasodilation below level of blockade, decreasing SVR (15-20%) leading to decreased preload and therefore CO (10-15%)
- venous dilation > arterial dilation
- If blockade is at or above T1-T4 the cardiac accelerators are blocked, leading to bradycardia
- Can result in profound hypotension
- Treatment:
- vasopressors
- volume load (15 ml/kg)- if pt can tolerate
- +/- vagolytic drug to treat bradycardia
What are the pulmonary effects of neuraxial anesthesia?
- Low levels of blockade will have minimal effect on MV, TV, RR, and dead space
- As the block ascends, accessory muscles to breathing will become paralyzed, causing the pt to feel like they can’t breath. Also decreases the ability to cough and protect the airway
- No direct respiratory effects excep those related to positioning unless high block
- Phrenic nerve at C3-C5
- Profound hypotension may cause ischemia of the central respiratory centers leading to respiratory arrest.
What are the GI effects of neuraxial anesthesia?
Renal?
- N/V (20%)- usually due to low BP
- Hyperparistalsis d/t unopposed parasympathetic activity
- Liver bloodflow depends on BP- maintain BP to avoid liver damage
- Renal bloodflow is autoregulated, no major effects
- bladder dysfunction
- urinary retention
- In no foley is present, avoid excessive fluids
What are the endocrine/metabolic effects of neuraxial anesthesia?
- blocks the stress response to surgery
- good for pts with CAD (must maintain perfusion)
- Catecholamine release may be blocked from the adrenal medulla
- Cortisol secretion is delayed
- shivering/altered thermoregulation with vasodilation
- important to keep pt warm!
What are the neurological effects of neuraxial anesthesia?
- CBF is maintained unless MAP <60 mmHg
- Manifested by N/V and if sufficiently decreased, will cause apnea and hypoxia
- decreased signals to Reticular activating System (RAS) will cause drowsiness
How do you position your patient for SAB or epidural?
- Lateral decubitus
- forehead to the knees
- thighs flexed to abdomen
- Sitting
- good for lower lumbar or sacral block
- improved midline anatomy
What do you do to get ready for a SAB or epidural?
- have pt hooked up to appropriate monitors
- suction
- oxygen delivery
- fluid bolus (500-1000 ml)
- Equipment for airway management and resuscitation are available
- emergency drugs drawn and available
- consider sedation prior to procedure
- identify landmarks
What are the common landmards for an epidural?
SAB?
- Epidural- see pic
- SAB- below level of spinal cord (L2-L5 interspaces)

What are the two different approach/techniques you can use when placing an epidural or SAB?
- Median (most common)
- the needle or introducer is placed midline, perpendicular to spinous processes, aiming slightly cephalad
- Paramedian approach
- indicated in pts who cannot adequately flex because of pain or whose ligaments are ossified
- the spinal needle is placed 1.5 cm laterally and with a slight cephalad direction to the center of the selected interspace

What layers do you go through when doing the midline approach?
***this WILL be a question!!
- Tripple S- I Love Epidurals
- skin
- subcutaneous tissue
- supraspinous ligament
- interspinous ligament
- ligamentum flavum
- epidural space
- dura mater
- subdural space
- arachnoid mater
- subarachnoid space
- pia mater
- spinal cord

How is the paramedian approach different from the median approach as far as what layers it doesn’t go through?
When is it useful?
- Misses the supraspinous and interspinous ligaments
- unable to use the spinous process as a guide
- Useful in thoracic epidurals or patients with narrow vertebral openings
What are the different types of needles that can be used for SAB?
- Pencil point needles (sprotte/Whitacre)
- designed to spread the dural fibers and help reduce the occurence of post dural puncture headache
- you will feel a distinct “pop” as it penetrated the dura
- better tip strength to minimize bending or breakage
- Side hole enables directional flow of anesthetic and reduces the possibility of straddling the dura
- tracks straight when advancing through the dura
- Cutting needles (Quinke)
- dural “pop” less obvious
- increased risk of wet tap
- introducer may not be necessary depending on pt size
- bevel mist be facing left/right in sitting position and up/down in lateral position to decrease risk of wet tap

What is the procedure for a SAB?
- identify anatomic landmarks
- clean area starting at center and moving out
- apply drape, wipe iodine from site with sterile gauze
- use 2 cc of 1% lidocaine to make wheal at selected space. Use this needle to feel around for spinous processes
- Pass a 17g introducer through wheal site, angled slightly cephalad, stopping in the ligamentum flavum. Ensure bevel is parallel to longitudinal fibers
- 25g choice needle inserted into introducer, passing through arachnoid and stopping when CSF is noted
- if no CSF flowing, rotate 90 degrees
- CSF is aspirated into syringe with LA
- dose is slowly injected, aspirate again after instillation
- all needles removed, patient repositioned
What interspace matches with the Superior illiac crests?
L4
What is the procedure for a paramedian approach for a SAB?
- Identify the edge of the superior spinous process
- skin wheal 1 cm lateral and 1 cm caudad to that point
- insert needle aimed 10-15 degrees medial and slightly cephalad
- if lamina contacted needle, walk needle off in a medial and cephalad direction
- After CSF obtained, coninue same technique as median approach
What is density?
specific gravity? of CSF?
Baracity?
What are the different ratios of LA:CSF?
- Density- the weight in grams of 1 cc of solution at a specified temperature
- Specific gravity- the ratio of the density of a solution to the density of water (temp constant)
- Specific gravity of CSF = 1.004-1.008
- Baricity- the density of a solution to the density of another substance
- LA:CSF
- hyperbaric- LA has higher density than CSF
- hypobaric- LA has lower density than CSF
- Isobaric- LA has same density as CSF
- LA:CSF
How can the specific gravity of a LA be altered?
Which baricity of LAs produce reliable blocks?
- Specific gravity of a LA can be altered by the addition of dextrose/water or CSF
- Reliable blocks produced by isobaric or hyperbaric solutions
Hyperbaric solution:
specific gravity:
How is it made?
- specific gravity > 1.11
- mix the LA with dextrose
- higher baricity allows the LA to settle in dependent areas
Hypobaric solution:
specific gravity:
how is it formed?
- Specific gravity <1.005
- mix the LA with sterile water
Isobaric solution:
specific gravity?
how is it made?
- specific gravity <1.006
- mix the LA with CSF
What factors affect the spread of the LA in SAB?
- baricity of the LA
- position of the patient
- concentration and volume injected
- level of injection
- barbotage/rate of injection
- quicker injection = wider spread; just give it slow to prevent major autonomic response
- direction and level of bevel
What should you consider when dosing a SAB?
- where the surgical site is
- length of procedure?
- should vasopressors or decadron be added to prolong effects?
- body size
- go lower on dosing an obese pt as they will have more spread
- Physiology
What determines the duration of a SAB?
- Rate of LA elimination
- by vascular absorption via subarachnoid and epidural blood vessels
- vasoconstrictors can prolong length of block
What are the different epidural techniques?
- Continuous catheter technique with Tuohy needle (laterally facing opening)
- Loss of resistance technique
- air or saline filled glass syringe
- steady pressure on the plunger while advancing the needle
- once in epidural space, resistance is gone and fluid is easily injected
- note needle depth
- advance catheter an additional 2-3 cm into epidural space (4-6 cm in parturients)
Where are the epidural insertion sites?
- thoracic
- lumbar
- caudal
describe the epidural space.
- widest point is L2 = 5 mm
- contains fat and blood vessels
- closed space
- medication and catheter deposited into potential space
What is the procedure for an epidural?
- At the desired spinous process, the spinal needle is advanced into skin w/the needle bevel parallel to longitudinal fibers
- will pass through: skin, subcutaneous tissue, supraspinous ligament, interspinous ligament, ligamentum flavum (will “pop”), epidural space
- ligamentum flavum depth from skin is 4 cm and is 5-6 mm thick at midline in lumbar region
How will you know you are in the right spot with your epidural needle in an elderly patient?
know based on needle depth. Probably will not be able to feel the “pop” in an elderly person.
What is a Caudal block?
What are the landmarks for a caudal block?
- Caudal block- delivery of LA to the epidural space via injection through the sacral hiatus
- Access via sacrococcygeal ligament and sacral hiatus
- use 22 or 23g needle
- Landmarks:
- Sacral cornu
- posterior superior iliac spines (S2)
- sacral hiatus
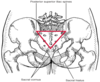
What is the procedure for a caudal block?
- Identify the sacral hiatus and PSIS
- insert needle in a slightly cranial direction through the hiatus at a 60 degree angle.
- advance until “pop” of sacrococcygeal membrane
- lower needle to a 20 degree angle and advance 2-3 mm to make sure bevel is in the caudal epidural space
- aspirate to confirm absence of blood and CSF and inject LA while feeling for inadvertent SQ injection with other hand
- there should be little resistance to injection
- **can inject 5 ml NS rapidly while palpating. If there is bulging, you are in wrong spot

What are the uses of caudal anesthesia?
What are the limitations?
- Uses:
- pediatric post-op pain control
- hyposadious (penis opening in wrong spot)
- inguinal hernia repair
- procedures of the perineal and sacral area
- limitations
- variable anatomy in adults (best in pt <7 yr old)
- high risk of injection into a venous plexus
- difficulty maintaining sterility should a catheter be used
How does a test does detect accidental intravascular injection?
subarachnoid injection?
- IV: increased HR and BP within one minute
- SA: cannot move legs within one minute
How does the volume and concentration of the LA affect the epidural block?
- Large volume of a dilute solution
- allows for wide segmental spread but with decreased sensory and motor blockade
- The quality and extend of the epidural block is dependent upon volume and concentration of the LA
How many m’s of LA do you use per segment you want blocked?
1.25-1.6 ml of LA per segment
What are the complications associated with spinal/epidural/and caudal blocks?
(15)
- hypotension
- bradycardia
- sudden cardiac arrest
- N/V
- unintentional IV injections
- unintentional intrathecal injection
- catheter shearing
- post-dural puncture headache
- high blockade
- inadequate blockade
- Neurologic complications
- bachache
- infections- septic meningitis
- urinary retention
- epidural hematoma
Post dural puncture headache:
incidence:
What is the physiology?
Who has higher incidence?
- Incidence: 1-4%
- The decrease in intracranial pressure combined with compensatory cerebral vasodilation will cause the brainstem to sag which stretches the meninges and pulls on the tentorium
- Fronto-occipital postural headache that occurs within one day to one week of spinal or epidural anesthesia
- Increased incidence:
- younger females
- larger needle size
- pregnancy
- using air for LOR
- cutting tipped needles perpendicular to meninges
- multiple puncture attempts
How is post dural puncture headache treated?
(7)
- bedrest
- hydration
- oral analgesics (NSAIDS)
- abdominal binder
- epidural saline injection
- caffeine
- epidural blood patch
What is an epidural blood patch?
How is it done?
How effective is it?
What are the side effects?
- Injection of pts blood into epidural space to form a clot over the puncture wound
- Procedure:
- aseptic autologous blood draw volume of 0-20 ml
- aseptic epidural injection of autologous blood into epidural space- at same level or more caudad to original insertion site
- Relief
- >90% effective
- if more than 2 attempts are made, hen other etiologies of HA should be ruled out
- Side effects:
- backache
- radicular pain (pain radiating to lower extremeties along spinal root
Epidural Hematoma:
What is the primary cause?
How does it presents?
Treatment?
- Primary cause is a coagulation defect
- Presents with numbness or lower extremity weakness
- Treatment:
- consult neurosurgery immediately one susptected (6-8 hours before there is a permanent injury)
- greater than 8 hours makes decompression less successful
What is the deal with LMWH and Heparin when planning to do an epidural?
- LMWH-
- hold 10-12 hours pre-placement of epidural
- hold 10-12 hours post surgical procedure
- Heparin-
- Can bae given 1-2 hours post SAB/epidural
What is the test dose of LA?
thanks Casey
- 3 ml of 1.5% lidocaine with 1:200,000 epi
- 15 ml lidocaine per ml
- 5 mcg epi mper ml
- total 45 mg lidocaine and 15 mcg epi
